
MRI is of value for the diagnosis of TOS: it identified a structure potentially responsible for TOS in 71% of the patients was capable for hypertrophy of the anterior scalene muscle (81%) and for diagnosing a cervical rib (100% sensitivity and 100% specificity) but it is time consuming and costly. Some authors state that CT scans can identify abnormalities in 30 to 60% of cases, but TOS caused by soft tissue is difficult to diagnose with CT. However, EMG cannot provide anatomical information regarding nerves and surrounding tissues, and the examination results are also affected by various factors. The insidious onset and slow progression of symptoms usually result in delayed diagnosis.Īt present, the diagnosis of TOS with the lower trunk compression of brachial plexus commonly relies on electromyography (EMG), CT and magnetic resonance imaging (MRI), in addition to medical history and clinical examinations. Neurogenic TOS is mainly caused by the lower trunk compression of brachial plexus (the C8/T1 roots) patients may experience pain, numbness, paresthesia, and motor weakness. 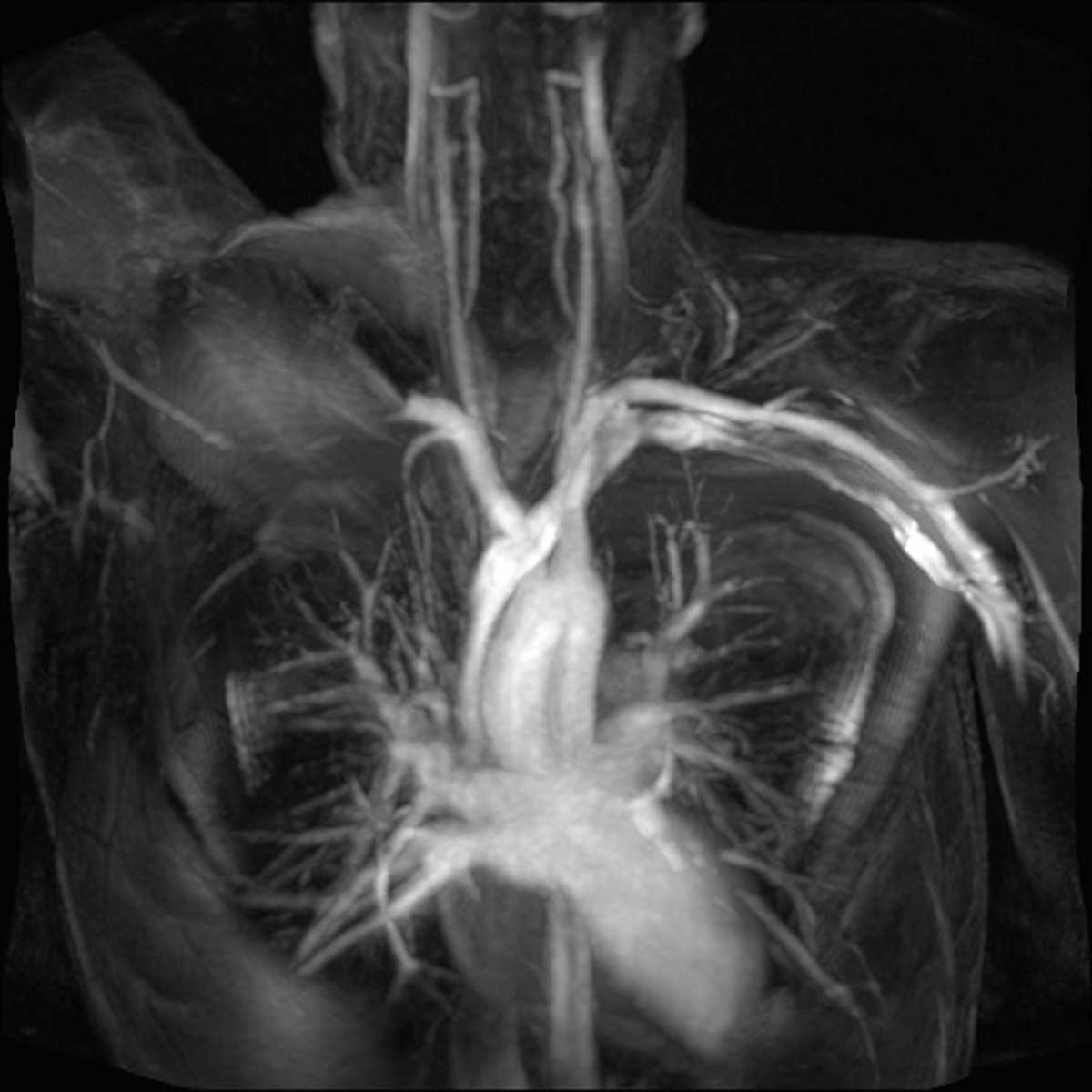
TOS is subdivided into neurogenic, arterial, or venous TOS based on the compressed structure, in which neurogenic TOS accounts for approximately 90% of cases. Thoracic outlet syndrome (TOS) is a group of diverse disorders involving compression of the nerves and/or blood vessels in the thoracic outlet region, including the subclavian artery, subclavian vein and trunks of the brachial plexus. TOS with the lower trunk compression of brachial plexus can be diagnosed accurately and reliably by high-frequency ultrasound. 
Surgical results showed that the etiological factors contributing to TOS were (1) muscle hypertrophy and/or fibrosis (100%) and (2) cervical ribs/elongated C7 transverse processes (20.7%). (3) Abnormal bony structures: cervical ribs or elongated transverse processes of the 7th cervical vertebra (C7). (2) Hyperechoic fibromuscular bands behind the compressed nerve (mostly the scalenus minimus muscle). Healthy side: 0.38 ± 0.06, P = 0.009), and the cross-sectional area of brachial plexus cords was markedly greater on the injured side than on the healthy side (0.95 ± 0.08 cm² vs. HFUS revealed focal thinning that reflected compression at the level of the lower trunk furthermore, the distal part of the nerve was thickened for edema (Affected side: 0.49 ± 0.12 cm vs. The HFUS features of TOS can be summarized as follows: (1) Lower trunk compression. Most cases had unilateral involvement (92.6%), mainly on the right side (66.7%). 
TOS occurred predominantly in females (70.4%). The imaging data were compared, and the pathogenesis of TOS was analyzed on the basis of surgical data. The ultrasound data of 27 patients who had TOS with the lower trunk compression of brachial plexus were collected and eventually confirmed by surgery. This study aimed to summarize the features of thoracic outlet syndrome (TOS) with the lower trunk compression of brachial plexus observed on high-frequency ultrasonography (HFUS). Thoracic outlet syndrome (TOS) with the lower trunk compression of brachial plexus (BP) is difficult to diagnosis.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
